Well, kids, here we are. The year is 2021 — nearly 2022 — and somehow I have a 2(!) year old.
And slowly but surely, a number of the insta-friends who had their donor-egg IVF (DEIVF) miracle babies around the same time as we did have started trying for (and in some cases already having) miracle #2. I feel bad for even admitting this, but it’s been making me a bit envious, if I’m honest.* And yet, despite being in the extremely fortunate position of having three more donor-egg embryos in the freezer, we haven’t quite managed to get back in the saddle ourselves for a number of reasons that I’ll get into now.
First off, it turns out that babies are incredibly poor sleepers. Apparently there are some people who can function on 4-6 non-consecutive hours of sleep a night, but I’m not one of them. I’ve been barely able to spell my own name, much less find the time/energy to consider adding another infant to the mix. Especially when this involves coordinating the logistics of an international embryo transfer.
Because despite having tackled one of the biggest obstacles to pregnancy (namely, having viable embryos) thanks to our egg donor, Marie, the practical details of another transfer are still non-trivial. Our embryos are at our clinic in Belgium, while we live several hours away in the Netherlands. For our first three DEIVF embryo transfers, I managed to convince a local Dutch clinic to do the monitoring (ultrasounds and blood tests) during the early part of the cycle so that we only had to drive to Belgium for the actual transfer. Unfortunately, the Dutch clinic we used before has said they will no longer help. This means I will either need to find another local clinic to do the necessary monitoring (no luck so far) or resign myself to making multiple long drives back and forth across the border.
Additionally, there’s the fact that I’m still breastfeeding MB. It’s only a little bit (and only before bed). Nevertheless, the official advice is that you must stop breastfeeding before a cycle since the prescribed hormones are transmitted through breast milk. I haven’t wanted to rush the weaning process, however, since — as a mom via donor eggs — the chance to breastfeed has been so extra special.
Small steps
Since we didn’t know what other steps would be needed prior to a new transfer attempt (eg. rejoining the waitlist, protocol changes due to my current use of hormone replacement therapy (HRT), etc), we made an appointment at our clinic a few months ago to ‘start the process’. In our horse analogy, this isn’t getting back in the saddle, exactly, but it is taking time to figure out where the heck you put the saddle last time you used it.
At the appointment, we learned I needed to redo my bloodwork for thyroid monitoring and a number of standard checks. We also filled out a metric ton of paperwork — approximately the same amount I imagine you’d need to fill out if you were acquiring a small nation state.
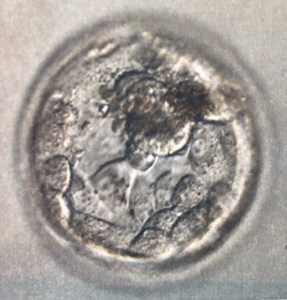
Excitingly, we got the great news that our remaining frozen embryos are good quality. (There was so much going on during our first few transfers that we couldn’t quite remember.) We have a 4BB and two 3BBs. These are all better grades than MB, who grew from a scrappy 3BC. That doesn’t guarantee any of them will work, of course, but the doctor seemed quite optimistic that we at least have a shot.

Lastly, we learned that there’s no waitlist to start, so it’s up to us (ie, whenever I’m ready to stop breastfeeding MB and sleep even less again). They sent us home with the prescriptions for the hormones, and instructions that I could simply start them as soon as I stop the HRT and start my period. Easy peasy.
Spoiler: It was not easy peasy
Reader, I had a gut feeling it would not be so simple. You see, I’ve been bleeding almost continuously on the HRT, which is an annoying but apparently not-unheard-of side effect. Between that and my post-menopausal ovaries, I was quite skeptical that I’d get my period after stopping the HRT (despite the doctor’s assurance it would come ‘within three days’). So after worrying uselessly about it for a few weeks, I staged my own test run by stopping the HRT and waiting to see what happened.
I waited one day. Two days. One week. Two weeks… Still no period. At that point, I was starting to feel the (very unpleasant) effects of stopping the HRT, so I gave up and started again, figuring I’d simply ask the doctor to clarify the protocol in such a circumstance. It may seem like a minor point, but I didn’t want to submit myself to the physical and emotional stress of strong fertility hormones and international trip logistics if the timing wasn’t right to start a cycle in the first place.
I emailed the clinic to clarify. I won’t bore you with the details of everything that followed, but the short version is that I spoke with three different other doctors/nurses at the clinic and got three different answers to this very basic question. As I was getting increasingly frustrated, I finally demanded that our doctor — who I had yet to hear from, and who I like and trust more than anyone else there — call me.
That’s when it came out that our doctor is not currently ‘there’…. As in, she’s missing in action. As in, they don’t know ‘if or when she’ll be back’. And when we said we hoped she was ok, they replied, ‘We do too.’
So to beat a dead (horse) analogy: we’ve found the saddle, we’ve dusted it off, but now the dang horse has gone missing.
xx
* This feeling of envy is itself difficult to reconcile with the deep-rooted notion that I should be grateful for what I already have. This is probably some form of post-infertility-trauma survivor’s guilt…but more on this incredibly cheery topic in another post!
Follow me on Instagram: @thebunlessoven